Aesthetics
Face
The most modern facial treatments help you look younger, more elegant and happier.
Body
Feel comfortable in your body and correct sources of discomfort.
Chest
Make your wish for a better appearance come true and restore your self-confidence with aesthetic correction.
Hair and scalp
Minimally invasive solutions for hair loss and a natural look.
Issues
Find solutions to some of the most common aesthetic problems.
Treatments
Surgery
Treatments

Hair and scalp mesotherapy
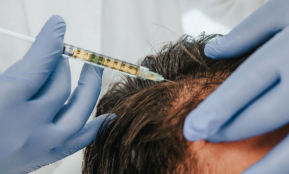
Thinning hair therapy with your own blood

Trichotest – DNA analysis of hair loss and baldness

Hair loss in women – causes and how to prevent it

Hair loss in men – causes and how to prevent it
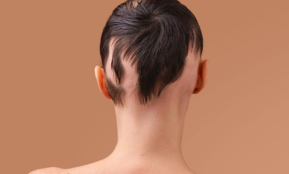
Alopecia – hair loss
FACE

BODY
Implantology Center
Different methods of solving the problem of missing one or more teeth.
Prosthetics
The most common solution in cases of functional or aesthetic tooth damage.
Aesthetic Dentistry
Harmonious tooth shaping and tooth color correction according to your wishes.
General Dentistry
Modern and timely diagnostics, treatment and dental hygiene are the key to the health of your teeth.
Issues
Find solutions to some of the most common aesthetic problems.
About us
Locations
Description of the procedure
Dermatoscopy or dermoscopy is a diagnostic method of observing changes on the skin with the help of a dermatoscope, an instrument that increases the field of view with polarized or non-polarized light, and its primary meaning is in the evaluation of pigment changes on the skin.
It is performed after a clinical examination, and allows observation of the epidermal and deeper structures of the upper dermis.
It helps the dermatologist to distinguish melanocytic from non-melanocytic changes, and its greatest significance is in the early diagnosis of melanoma.
Melanoma is a malignant skin tumor that can arise from a malignant transformation of a mole or as a change in the skin that was not there before.
Melanoma becomes a potentially curable cancer if detected early enough and treated at an early stage, and unlike other cancers, it can be relatively easily detected through regular skin examinations.
Dermatoscopy is an aid in distinguishing different tumors on the skin (keratoses, dermatofibromas, hemangiomas, basal cell, or planocellular carcinomas and other changes).
A dermatoscopic examination helps us diagnose the type of change and determine when a particular change needs to be removed.
Digital dermatoscopy allows monitoring of suspicious moles that change over time. During each examination, photographs are stored and compared with previous ones, and in the event of certain changes in the observed lesion, an indication is set for its removal.
Candidates
Digital dermatoscopy is an important monitoring method in people with an increased risk of developing melanoma, namely people who have:
- syndrome of atypical (dysplastic) nevi
- a history of melanoma or other skin cancer (or someone in their family)
- a large number of moles on the body
- fair-skinned and generally very sensitive to sun exposure (red-haired people, with freckles)
- sunburns that occurred in childhood and adolescence
- Chronic exposure to UV radiation due to profession or hobby
If you notice changes in your mole, such as asymmetry, irregular edges, a change in color or an increase in the diameter of the mole, or if it bleeds or itches, be sure to consult a dermatologist.
It is recommended to have moles checked once a year, and more often for people at increased risk, as advised by a dermatologist.
Preparation
Digital dermatoscopy does not require special preparation. Before the examination, it is advisable to come with clean skin, without creams, oils and self-tanning products. If the patient uses some local preparations, it is necessary to mention them to a specialist in dermatovenerology.
Procedure progress
At the Bagatin Polyclinic, we use the most advanced dermatoscope from the renowned German company Visiomed AG, which specializes in medical diagnostics.
It is an integrated system for early detection of skin cancer, and is specially designed to fulfill all the most important aspects of skin examination and visualization.
Due to its precision, it is one of the most valued devices for the diagnosis of skin cancer, which is confirmed by numerous scientific awards and prizes.
Through the synergy of various diagnostic modules, the dermatoscope enables a standardized examination of suspicious skin changes, as well as detailed personal photo documentation and monitoring of moles over time.
The device itself magnifies the skin from 15 to 120 times with the help of calibrated optics to ensure consistent mole analysis every time.
A digital dermatoscope enables the capture, annotation, storage and transfer of dermatoscopic photographs, as well as clear visualization and analysis of suspicious lesions, for both clients and doctors.
The advantage of examining moles with the help of a digital dermatoscope:
- Standardized mole examination at each check-up
- Monitoring the development of moles over time – comparing the appearance of moles with previous ones
- In-depth analysis of the structure, shape and color of moles
- Photo documentation – helps to decide on the need for surgical removal of moles
Recovery
Examination using a digital dermatoscope is completely painless, and you can return to activities after the examination. If the dermatologist determines during the examination that it would still be good to remove a mole or skin change, there is no need to worry.
Our Polyclinic offers as many as three methods of removing moles and other benign changes, namely surgical, laser and radiofrequency removal.
Surgical method It involves removing moles with a surgical knife.
The mole must be completely removed, meaning the surface part and the part that is under the skin.
When it comes to a smaller mole, the wound is sutured directly, and if the mole is larger, local flaps from the side or free skin grafts are used.
The post-operative treatment after the procedure lasts about seven days, and in the first days after the removal of moles, the places where they were must be bandaged.
After the stitches are removed, the treated areas are treated with prescribed creams for the next few weeks to help reduce the scar.
The laser method with the help of the Erbium laser is the simplest method for removing moles and other skin changes.
In most cases, anesthesia is not required for their removal.
It involves the use of laser light, the beam of which is directed directly at the mole to heat it and then destroy it.
It is painless, does not require cutting or stitching the skin.
Also, with laser mole removal, there is less chance of scarring than with other removal techniques.
After the laser treatment is complete, a scab forms where the mole once was.
This scab usually lasts for about two weeks and then falls off.
It is important to note that during laser treatment, the skin change is completely removed at the microscopic level, and there is no possibility to send the treated tissue to a pathologist for analysis to establish a definitive diagnosis.
With Ellman radiofrequency, only the change on the skin is removed, after local anesthesia which is injected with a very thin needle under the growth itself.
Immediately after treatment, a non-bleeding skin wound appears at the site of the growth, the same size as the removed growth.
A scab then forms, and after 7-10 days a fresh layer of skin forms, which over time blends back into the surrounding skin.
Precautions
There are no contraindications for a dermatological examination. After the dermatological examination, you can return to your usual activities.
Price
In cooperation with banks, Bagatin Polyclinic provides the option of paying in installments, as well as interest-free payments up to a certain number of installments.
You can find out more about payment methods and the cost of the examination in the current price list of the Bagatin Polyclinic:
They said about us...
They said about us...
Your
Frequently asked questions
Contact us
Contact us with confidence.
By filling out this form, our call center will contact you within 24 hours to arrange your appointment. We keep all information you provide us with in the strictest confidence.
Phone:
E-mail:

















